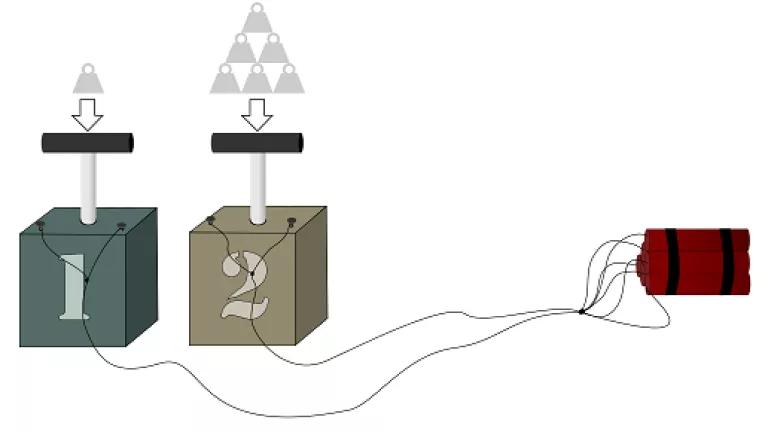
Imagine for a moment that you have two, Wile E. Coyote-style detonator boxes attached to a single bundle of TNT. One detonator box has one weight pushing the handle down while the other has six. Which box do you think would detonate the dynamite first?
Box number two, right?
What if you were to add one more weight to each of the handles? Box number two would still ignite the dynamite faster than box number one.
Now, what if we swapped out the dynamite for a negative health outcome and the detonator boxes for people? Box number one might represent a person that lives in a safe, clean neighborhood, with access to education, financial resources, green spaces, and healthy foods. Box number two might be a person that lives in a violent, noisy, poverty-stricken neighborhood, with limited access to fresh foods and constant exposure to multiple sources of pollution. If both of these boxes represented children, and the additional weight added to their handle was exposure to lead, would one be more likely to experience the neurodevelopmental impacts of that lead exposure? A recent study in Human and Ecological Risk Assessment sheds some light on this question.
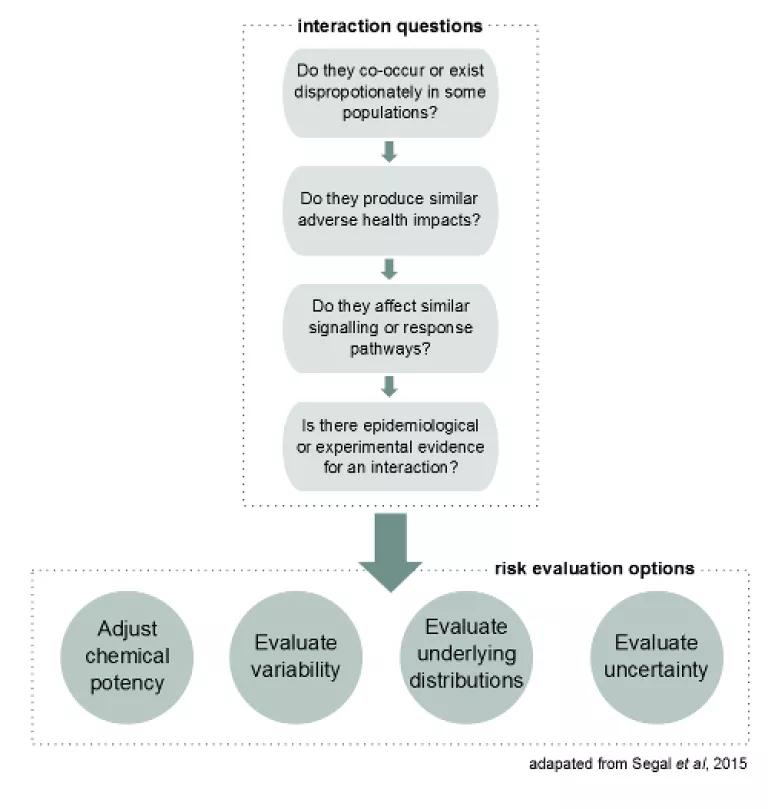
In their study, "A Conceptual Framework for Evaluating the Interaction of a Chemical and Nonchemical Stressor in Human Health Risk Assessments: A Case Study for Lead and Psychosocial Stress", Segal et al. posed two primary questions. First, is there an interaction between psychosocial stress (a non-chemical stressor) and lead (a chemical stressor)? Second, if lead (chemical stressor) and psychosocial stress (non-chemical stressor) do interact, how can that information be incorporated into a risk evaluation? To answer these questions, the authors developed a framework (see below), evaluated nationally-representative datasets, and performed an extensive literature review.
Is there an interaction between the lead and psychosocial stress?
According to the study authors, in order for a chemical and non-chemical stressor to exhibit an interaction, four criteria should be met. First, the chemical and non-chemical stressors need to disproportionately co-occur or exist in certain subgroups within the population. Second, the chemical and non-chemical stressors need to lead to a similar adverse health outcome. Third, the chemical and non-chemical stressors should impact similar signaling of response pathways that lead to the negative health outcome. Finally, epidemiological and/or experimental evidence should demonstrate that the chemical and non-chemical stressors interact.
The relationship between low socioeconomic position, psychosocial stress, and negative health outcomes has been studied for decades, if not centuries (see Lynch and Kaplan for more details). Low SES individuals are more likely to suffer from cardiovascular diseases, premature mortality, and a myriad of other ailments, due, in part, to the chronic stress associated with poverty. In addition to suffering from increased amounts of stress, low SES groups are also more likely to be exposed to lead through contact with lead paint and legacy soil contamination from leaded gasoline. Children in low SES groups have been shown to have higher blood lead levels than their more affluent counterparts in both the U.S. and Mexico.
In addition to co-occurring in the same subpopulation, both lead and psychosocial stress can impact neurodevelopment via the hypothalamic-pituitary-adrenal (HPA) axis. The HPA axis helps regulate our response to stress and is formed by various pieces of the nervous and endocrine systems (see Smith and Vale for more details). Psychosocial stress and lead can both alter the levels of corticosteroids (chemicals that transmit signals within the HPA axis) in human and animals, which can lead to improper functioning of the hippocampus - a region of the brain involved in memory and learning.
Finally, evidence from human and animal studies has shown that low social position can enhance the neurodevelopmental impacts of lead. A prospective cohort study by Bellinger et al found that while children of all social classes showed declines in cognitive development at the highest blood lead levels, only children with low social status showed declines in mid-level exposure to lead. In animals, several studies (see Schneider et al., Guilarte et al., and Cao et al.) have shown that the neurodevelopmental effects of lead can be altered based upon the living environment of a rat (e.g. an impoverished - lack in stimuli or companions - or enriched environment).
Though more research could aide in helping researchers fully understand the interaction between lead and psychosocial stress at the biological and social levels, a large body of scientific evidence suggests a likely association.
How can the association between exposure to lead and psychosocial stress be incorporated into a risk evaluation?
The idea of incorporating non-chemical stressors into evaluations of risk is not a new one. In its 2003 Framework for Cumulative Risk Assessment, USEPA defined cumulative risk assessment as "an analysis, characterization, and possible quantification of the combined risks to health or the environment from multiple agents or stressors", with multiple agents and stressors including both chemical and non-chemical forms. In the 2009 National Academies of Sciences report Science and Decisions, the Committee on Improving Risk Analysis Approaches noted that social and economic factors could increase individual vulnerability to the effects of environmental chemicals and that the appropriate inclusion of non-chemical stressors in cumulative risk assessment could "lead to more informative assessments and correspondingly better decisions".
Segal et al. proposed several ways in which chemical stressor/non-chemical stressor interactions might be incorporated into a cumulative risk assessment. First, the potency of a chemical could be adjusted to account for increased toxicity related to the non-chemical stressor. That is, the thresholds at which a chemical is thought to cause harm could be lowered to account for populations with high levels of the non-chemical stressor.
Second, the chemical stressor/non-chemical stressor interaction could be used to evaluate variability within the population. If, for example, low SES populations respond differently to lead than high-SES populations, the variability in the population should be explored and accounted for.
Third, the chemical stressor/non-chemical stressor interaction could be used to evaluate the effect on existing distributions for the chemical stressor. In the lead example, this might mean investigating the role that psychosocial stress might play in lowering IQ (a known outcome of lead exposure). If psychosocial stress has the ability to alter IQ, this could strengthen the connection between neurodevelopmental impacts and stress and highlight the importance of including highly stressed populations in the risk analysis.
Finally, the chemical stressor/non-chemical stressor interaction could help risk assessors evaluate uncertainty. If there is evidence of disproportionate exposure to a chemical in a stressed population, and possible links between the chemical and psychosocial stress, psychosocial stress could be an important source of uncertainty in the risk evaluation.
The appropriate incorporation of non-chemical stressors into risk evaluations represents an important step toward fully protecting human health from the potentially harmful impacts of environmental chemicals. Though the Segal et al. paper is an early step in the incorporation process, the framework provides an additional platform upon which regulators and other researchers can shift the "one-chemical-at-a-time" risk assessment paradigm to a more cumulative approach - making sure that no matter how many "weights" are on our particular handle, the risk assessment process is protective for us all.
