It's Official - Again: CDC report on antibiotic resistance warns of "potentially catastrophic consequences of inaction"
This is not how it was supposed to be. Seventy years after the discovery of penicillin revolutionized modern medicine, infections aren’t supposed to be killing again. But as the Centers for Disease Control and Prevention (CDC) explained in a report on the antibiotic resistance crisis today, this is our new reality.
According to the report, every year, at least 2 million people in the U.S. are hobbled by serious antibiotic resistant bacterial infections, 23,000 people die of those infections, and many more die from conditions caused by complications from those infections.
I recently joined some Pennsylvania medical doctors as they alerted one of their Senators to this public health crisis. These doctors are working on the front lines and see firsthand the disaster that is before us. One doctor mentioned a patient who had hurt his leg from falling. The leg became infected and none of the medicines they tried worked. Eventually, the doctor was left with one remaining antibiotic that came with serious side effects. He presented his patient with this harrowing choice: take the antibiotics and be on dialysis for the rest of your life, or we amputate your leg.
And that is what we have come to. Amputations are sometimes the only hope for treating infections caused by antibiotic resistant bacteria as they once were before the advent of antibiotics.
We also risk losing other major medical advances dependent on antibiotics, including cancer chemotherapy, complex surgery, organ and bone marrow transplants, dialysis and treatment of diseases like rheumatoid arthritis.
The CDC report looks at the different contributors to the problem of antibiotic resistance. Yes, the misuse of antibiotics in humans is part of the problem, and in response many doctors and hospitals have developed antibiotic stewardship programs across the country to address it. But to fully overcome this threat, we need to put a stop to all inappropriate antibiotic uses causing resistance, meaning we cannot ignore the rampant misuse of antibiotics in livestock.
The math is easy enough. Almost 80 percent of the antibiotics sold in the U.S. are used for livestock.
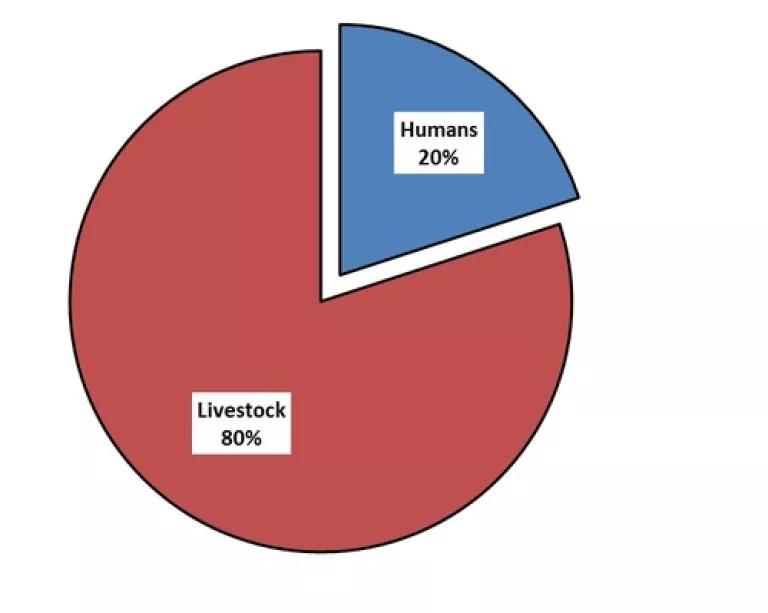
And the vast majority of those antibiotics are estimated to be used on animals that aren’t even sick. Instead, these healthy animals are given a low dose of antibiotics day after day to help them grow faster or to ward off diseases caused by the fact that they are living in unsanitary, cramped conditions on these factory farms. This routine dosing provides the perfect environment to breed superbugs by killing off just the bacteria that are susceptible to the antibiotics and leaving those that are stronger behind to reproduce and make more, stronger bacteria. And when these bacteria travel off the farms and enter our communities, then we are the ones faced with the Sophie’s choice for treatment.
The CDC recommends that we need to improve how we are using antibiotics, noting that “these drugs should only be used to treat infections.” This includes improving how antibiotics are used in livestock since the use in animals also contributes to the emergence, persistence, and spread of antibiotic resistant bacteria.
But from all appearances, we can’t count on the Food and Drug Administration (FDA) to make these necessary improvements.Despite recognizing this problem more than 35 years ago, the FDA’s only real action has been to propose guidelines on how antibiotics should be used in livestock that are not only voluntary, but also leave gaping loopholes that allow antibiotics to still be used on healthy animals under the guise of “disease prevention.”
But as luck would have it, there are bills in Congress now that would do just that: allow important antibiotics to be used only on sick animals (such as S. 1256 and H.R. 1150).
The CDC also recommends that we move to fill knowledge gaps about the use of antibiotics in livestock. And again, there are bills in Congress that would take an important step towards collecting and getting that information out publicly (S. 895 and H.R. 820).
Today’s report is yet another wake-up call that we need immediate action to reclaim these important antibiotics. We can’t let the industrial livestock and pharmaceutical companies keep hitting the snooze button on the alarm that’s sounding and thus exhaust one of the most important medical advances of our modern medical era. With better laws, more transparency, and healthier business practices, we may be able to avoid going back to a pre-antibiotic era.
Updated: Check out my colleague Carmen Cordova's blog here for other studies linking livestock and hospital infections. Also, updated to add link to the CDC teport above.
