Drinking In the Heavy Metal
Thanks to the Flint water crisis, the city’s kids could experience terrible, long-lasting consequences from lead exposure.
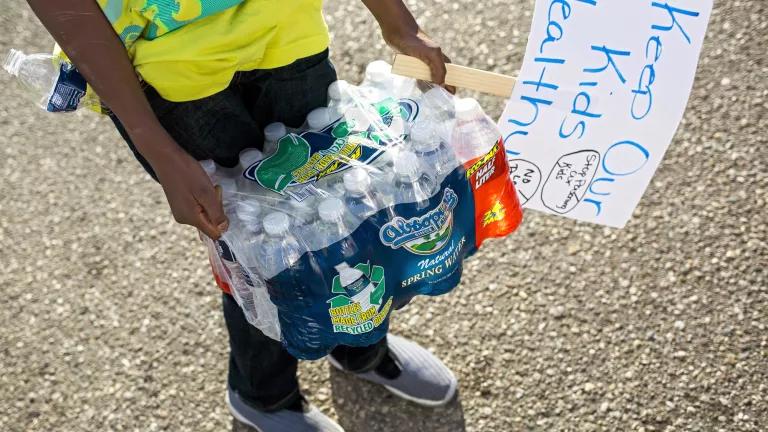
Danny Miller/The Flint Journal-MLive.com via AP
I met Melissa Mays in downtown Flint, Michigan, at a coffee shop called Café Rhema. A sign in front reads: “Serving Pure Water. Our water is filtered using reverse osmosis.” That’s why Mays asked me to meet her there. The city’s water hasn’t been safe to drink for nearly two years, though residents have known about the problem for only a matter of months. Commercial filters like the café’s that remove lead from the water can cost several thousand dollars, and those you would install below your sink cost several hundred. Only a handful of Flint's businesses and homeowners can afford them. Mays and her husband, Michael, plan to use this year’s tax return to buy filters for their house, where they live with their three children, Caleb, 17, Christian, 12, and Cole, 11.
Mays, who has long, straight, light-brown hair and hazel eyes, calmly sips her latte as she tells me her horror story. She suffers from autoimmune problems, seizures, polyps in her colon, cirrhosis of the liver, and diverticulitis, an infection in her digestive tract that Mays describes as an old person’s problem. She is 37. Her ailments started more than a year and a half ago and likely stem from drinking water polluted with high levels of heavy metals like copper, aluminum, tin, chromium, and lead.

Before Mays took a leave of absence in January to tend to her health, she had a full-time job doing PR and marketing for radio stations, and in her spare time, she did the same thing for hard rock bands. “I used to be the metal lady,” she says of her work promoting those bands. Now she’s a metal lady for a different reason, and she’s suing the city of Flint over it. NRDC (disclosure), the American Civil Liberties Union of Michigan, and the group Concerned Pastors for Social Action are co-plaintiffs in the case.
The Mays family had been consuming lead-laden water for a year when concerns about their rashes and hair loss led them to stop drinking from the tap and eventually to the pediatrician’s office. At the time of the boys’ testing, none had high blood lead levels, but the whole family was (and remains) anemic, a sign of lead exposure. All three boys now have trouble concentrating at school and complain of bone pain. Not all of their ailments are symptoms of lead exposure; some are likely due to the other contaminants in the water. But it’s the lead that could take the biggest toll overall.
* * *
Ingesting lead can result in irreversible damage to a child’s brain. The U.S. Environmental Protection Agency doesn’t step in unless concentrations are higher than 15 parts per billion (ppb) in 10 percent of sampled taps. Soon after April 2014, when the city of Flint switched to water from the Flint River, many of the city’s 100,000 residents have been drinking lead at much higher concentrations than that. The effects are undetectable at first, but as children grow, they can develop learning disabilities, developmental delays, speech impairments, attention and hyperactivity disorders, and lower IQs. They may have behavioral issues, and they face elevated risks for teen pregnancy and criminal conduct. For these reasons and others, the Centers for Disease Control and Prevention says there’s no acceptable level of lead exposure.
“When pediatricians hear ‘lead,’ we absolutely freak out,” Mona Hanna-Attisha, a pediatrician at Flint’s Hurley Medical Center who found high lead levels in the city’s children, told me in October. “Lead is one of the most damning things you can do to a child in their entire life-course trajectory.” It can also cause health problems in adults. When preparing for a reporting trip, I don’t normally pack a case of bottled water in my car. For this one, I made an exception.
For the kids of Flint, though, it’s already too late. Lead has made its way into their bodies, where it may have permanently damaged the neurons in their still-developing brains. I came here to see what the community is doing now to try to prevent this already terrible problem from getting worse years down the line.

The experts say the most important thing is getting those kids off lead as soon as possible. The half-life of lead in blood is 20 to 30 days. After its trip through the bloodstream, it begins settling in bones. The only way to remove the toxin from the body is through chelation therapy, but this is not recommended unless someone’s lead level is at least 45 micrograms per deciliter of blood (µg/dL) because of the treatment’s potential to damage the kidneys.
When Hanna-Attisha conducted her study on blood lead levels in Flint’s kids last summer, she found that most were lower than 10 µg/dL But while these kids are not candidates for chelation, they are not in the clear. Blood level tests take just a snapshot of what’s happening in the body at one moment in time, and studies show that a bump of just 1 µg/dL can cause cognitive, behavioral, and health problems. Other research shows some of the steepest decreases in IQ occur when µg/dL levels are below 10, says Jessica Reyes, a health economist at Amherst College in Massachusetts who has studied lead for 15 years. For every microgram of lead a child gains, he or she can lose three-fourths of an IQ point. One study found that those with a childhood blood lead average over 6 µg/dL have an increased risk for criminal behavior as adults (with risk rising more than 25 percent for every 5 µg/dL increase).
At one point, the water coming into LeeAnne Walters’s home had a lead concentration of more than 700 ppb. “The levels of lead in her house were astronomical. They way exceeded toxic waste levels,” says Hanna-Attisha. Gavin, one of Walters’s four-year-old twins, had a blood lead level of 6.5 µg/dL when he was tested last summer, and he’s since developed a speech impediment. Since the age of two, Gavin had been pronouncing his cousin’s name perfectly. Now he seems to be able to refer to Jordan only as Gordon.
“Every kid is different,” says Hanna-Attisha. “Not every kid is going to have every problem.” Still, the more lead a child ingests, the more likely that health and behavioral issues will crop up.
* * *
For the 40 percent of Flint’s residents who live below the poverty line, getting clean water isn’t as easy as buying a reverse-osmosis filter like Café Rhema or picking up a $20 case of Poland Spring at the store. If the city can stop lead exposure right now, it may not see the very worst societal effects, like high crime, says Kim Dietrich, an epidemiologist who’s been investigating lead and brain development through the Cincinnati Lead Research Study at the University of Cincinnati for the past 35 years. The children who have elevated blood lead levels for a long time are the ones who have the worst behavioral deficits, he says, “so time is a factor.”
But according to Reyes, even low levels of lead exposure can lead to criminal behavior down the road. “The effects do last, even if someone’s lead level goes down,” she says. That doesn’t necessarily mean every exposed kid becomes a criminal, but the likelihood goes up if he or she was exposed before turning three. Whatever may lie ahead, Flint’s parents, teachers, and pediatricians want to be prepared. And over the short term, that planning comes in the form of 12,000 gallons of milk.
A semitrailer truck rolled into the parking lot of the Food Bank of Eastern Michigan three weeks ago carrying thousands of gallon jugs of milk. The delivery was part of an initiative led by the Hurley Medical Center and Michigan State University. Providing foods high in calcium, iron, and vitamin C is crucial to reducing how much lead gets into a child’s blood system. And keeping them well fed is critical, too. A child with an empty stomach will absorb two to ten times more lead from the environment than one who, say, had breakfast.
In addition to the milk delivery, the initiative offers a weekly lead-free cooking class at the city’s year-round farmers’ market, found in the heart of town, for anyone who’s interested. Also in the works is a plan to bring psychologists, pediatricians, epidemiologists, and other medical experts together to monitor the children and help address any problems that develop over time. What they need, Hanna-Attisha says, are more early-literacy programs (some existed before the water crisis), universal preschool, good nutrition, and educated teachers who can help mitigate some of the damage.
When pediatricians hear ‘lead,’ we absolutely freak out.
“We cannot sit back and wait to see how bad it is,” she says. “We can’t reverse it, but we can lessen the impact.” Ultimately Hanna-Attisha would like to create a public health model in case a lead disaster like Flint’s should happen again.
Of course, Flint isn’t the first lead pipe crisis. Such crises have been happening for at least the last 150 years, writes Werner Troesken in his 2008 book The Great Lead Water Pipe Disaster. (“It was my Christmas reading,” says Hanna-Attisha.) In recent history, Washington, D.C., had twin water disasters that poisoned thousands in 2001 and 2010. The exposed children in those cases are still fairly young, so the long-term impacts from the two incidents are yet to be determined. We have learned that pregnant women who drank D.C.’s tainted water suffered a higher rate of miscarriage.
Most of what’s known about the toxin’s effect on children is from lead found in paint and soil, a result of automobile exhaust. In the 1970s, the average U.S. blood lead level was a whopping 12.8 µg/dL. After Congress banned the heavy metal from gas, levels plummeted to 2.8 µg/dL by 1991. Over that time frame, the proportion of 1- to 5-year-old children with blood lead levels of 10 µg/dL or higher dropped from more than 88 percent to just below 9 percent.
“We were fine,” says Reyes of her generation, which grew up when the toxin was pervasive in the environment. “But we also could have been better. We just didn’t know it.” The more scientists study lead’s impacts, she says, the more harm they see. But it’s nearly impossible to measure a child’s lost potential.
* * *
Cassie Parkos was just nine months old in 1990 when her blood lead tests came back at 33 µg/dL. Her family lived in an old house in Everett, Massachusetts, and they’d been giving her powdered formula mixed with warm tap water every day for three months. Her father, Chuck, now the chair of the pathology department at the University of Michigan’s medical school, tested their water. Its lead concentration was 500 ppb, 200 ppb less than the water in the Walters home. The Parkoses stopped drinking the water immediately and eventually moved out. As an infant, Cassie underwent chelation therapy, and her blood lead fell to more acceptable levels over her two years of treatment.
Cassie went on to excel in school, and in 2015 she earned a master’s in mechanical engineering from the University of Cincinnati. Now, at 26, she’s an aerospace engineer at GE. Her mom, Nickie, says, “She’s a genius.”
Nickie Parkos became an advocate for better lead detection after her child was exposed to the neurotoxin, as have Mays and Walters. Mays started a group called “Water You Fighting For?” and began recording data on thousands of children and pregnant mothers in Flint, mapping their addresses and health issues on a spreadsheet. In her spare time, she distributes bottled water to halfway houses, nursing homes, and a dozen day care centers.
“There is no price you can put on my kids’ future. My kids were going on this awesome path, they were working their butts off, and now they hate school,” says Mays. “They forget things…. They’re having a hard time with it. I’m watching my kids struggle, and there’s nothing I can do to help.” But she’s certainly going to try.
This article was originally published on onEarth, which is no longer in publication. onEarth was founded in 1979 as the Amicus Journal, an independent magazine of thought and opinion on the environment. All opinions expressed are those of the authors and do not necessarily reflect the policies or positions of NRDC. This article is available for online republication by news media outlets or nonprofits under these conditions: The writer(s) must be credited with a byline; you must note prominently that the article was originally published by NRDC.org and link to the original; the article cannot be edited (beyond simple things such grammar); you can’t resell the article in any form or grant republishing rights to other outlets; you can’t republish our material wholesale or automatically—you need to select articles individually; you can’t republish the photos or graphics on our site without specific permission; you should drop us a note to let us know when you’ve used one of our articles.
An Ally in the Fight for Safe, Affordable Drinking Water for All
Fighting the Tide of Watered Down Justice
What Can We Do to Fix the Drinking Water Problem in America?